Current Suspected Overdose Deaths in Delaware for 2024: Get Help Now!
Find school water testing results and additional resources
Attention Medicaid Participants: Eligibility Renewals Restarted April 1, 2023
Lyme disease is the most common vector-borne disease in the United States with approximately 30,000 new cases reported each year.
Lyme disease gets its name from a small coastal town in Connecticut called Lyme. In 1975, a woman brought an unusual cluster of pediatric arthritis cases to the attention of Yale researchers. In 1977, the Yale researchers identified and named the clusters “Lyme arthritis." In 1979, the name was changed to "Lyme disease," when additional symptoms such as neurological problems and severe fatigue were linked to the disease. In 1982 the cause of the disease was discovered by Dr. Willy Burgdorfer. Dr. Burgdorfer published a paper on the infectious agent of Lyme disease and earned the right to have his name placed on the Lyme disease spirochete now known as Borrelia burgdorferi.

The BLAST Program was adapted by Delaware Public Health from the Ridgefield Connecticut Program to raise awareness of the most effective Lyme disease prevention practices, as well as to educate the community about the early signs and symptoms of Lyme and other tick-borne diseases to promote timely diagnosis and treatment.
^ ^^^^^^^^
Click Kids Korner for resources and fun activities!

Upload a photo of the tick and get information on the tick species! Knowing what species of tick has attached to you, a family member, or a pet will help determine whether you may be at risk for a tick-borne disease.
Delaware is among the top 10 states with the highest incidence rates in the United States.
| YEAR | STATEWIDE TOTAL NUMBER OF CASES* |
NEW CASTLE COUNTY |
KENT COUNTY |
SUSSEX COUNTY |
STATEWIDE INCIDENCE RATE1 |
|---|---|---|---|---|---|
| 2022 | 385 | 253 | 64 | 68 | 64 |
| 2021 | 354 | 250 | 40 | 64 | 65 |
| 2020 | 355 | 249 | 43 | 161 | 35.97 |
| 2019 | 641 | 437 | 86 | 136 | 65.83 |
| 2018 | 520 | 302 | 87 | 131 | 53.77 |
1Cases/100,000 based on population data from the US Census Bureau
*As per the CDC Case Classification Criteria-Please note that the CDC case classification for Lyme Disease changed in 2022
The Lyme disease bacterium, Borrelia burgdorferi, is transmitted to animals and humans through the bite of an infected blacklegged or deer tick. Immature ticks are very tiny and can be difficult to see which can increase the possibility of undetected tick exposures. The ticks that transmit Lyme disease can occasionally transmit other tickborne diseases as well like Powassan virus, babesiosis, and anaplasmosis.
There is no evidence that Lyme disease is transmitted from person-to-person. For example, a person cannot get infected from touching, kissing or having sex with a person who has Lyme disease. Humans most often acquire Lyme disease in the spring and summer months when they enjoy outdoor activities.
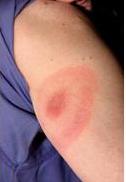
The Lyme disease bacterium can infect several parts of the body which can cause different symptoms at different times. Symptoms of Lyme disease can be nonspecific and may resemble other diseases. If you think you have Lyme disease it is important that you contact your healthcare provider. Follow this link for a printable poster of common symptoms.
Untreated infections can lead to a variety of symptoms, some of which can be very serious and debilitating. These symptoms can include:
DiagnosisDiagnosis is based on symptoms, physical findings (i.e., bull’s – eye rash, facial palsy or arthritis) and a history of possible exposure to ticks. Validated laboratory tests are available to assist the clinician with the diagnosis. Laboratory testing is not recommended or necessary when a patient develops the characteristic bulls-eye rash. Lyme disease can be difficult to diagnose. Not all patients with Lyme disease will develop the characteristic bulls-eye rash and tick exposures often go undetected. |
Most cases of Lyme disease can be cured with a few weeks of antibiotics taken by mouth. Depending on symptoms, some patients may require a second course of antibiotic therapy. Patients with certain neurological or cardiac forms of illness may require intravenous (IV) antibiotics.
A small percentage of patients with Lyme disease have symptoms that last months to years after treatment with antibiotics. These symptoms can include muscle and joint pains, arthritis, cognitive defects, sleep disturbance, and fatigue. The cause of these symptoms is not known. There is some evidence that they result from an autoimmune response, in which a person’s immune system continues to respond even after the infection has been cleared.
The Centers for Disease Control and Prevention (CDC) initiated Lyme disease surveillance in the United States in 1982. Lyme disease became a reportable condition in Delaware in 1989 under the Regulations for the Control of Communicable and other Disease Conditions which made Lyme disease, as well as many other diseases and conditions, reportable to the Bureau of Epidemiology in Delaware Division of Public Health (DPH).
In turn, DPH submits weekly data regarding all reportable diseases to CDC. CDC is then able to publish weekly reports and annual summaries in the Morbidity and Mortality Weekly Report (MMWR). The data in the weekly MMWR are provisional, based on weekly reports to CDC by state health departments.
For surveillance purposes, a case of Lyme disease in Delaware is defined according to the CDC/Council of State and Territorial Epidemiologists (CSTE) case definition.
The Bureau of Epidemiology in DPH utilizes the Delaware Electronic Reporting and Surveillance System (DERSS) to automatically receive positive laboratory results from major commercial laboratories on all reportable diseases, including Lyme disease. Additionally, all acute care hospitals in Delaware submit reportable disease reports electronically into DERSS.

Office of Infectious Disease Epidemiology
24/7 Emergency Contact Number: 1-888-295-5156
![]() Please note: Some of the files available on this page are in Adobe PDF format which requires Adobe Acrobat Reader. A free copy of Adobe Acrobat Reader can be downloaded directly from Adobe . If you are using an assistive technology unable to read Adobe PDF, please either view the corresponding text only version (if available) or visit Adobe's Accessibility Tools page.
Please note: Some of the files available on this page are in Adobe PDF format which requires Adobe Acrobat Reader. A free copy of Adobe Acrobat Reader can be downloaded directly from Adobe . If you are using an assistive technology unable to read Adobe PDF, please either view the corresponding text only version (if available) or visit Adobe's Accessibility Tools page.